|
Among the features cited for CBT nonadherence are the reported social isolation derived from lack of flexibility, boredom from imposed wakefulness during-re-entrainment, and rigidity of the sleep schedule often incompatible with working hours. Even when patient motivation is intact, aspects of CBT can lend patients to drop-out. 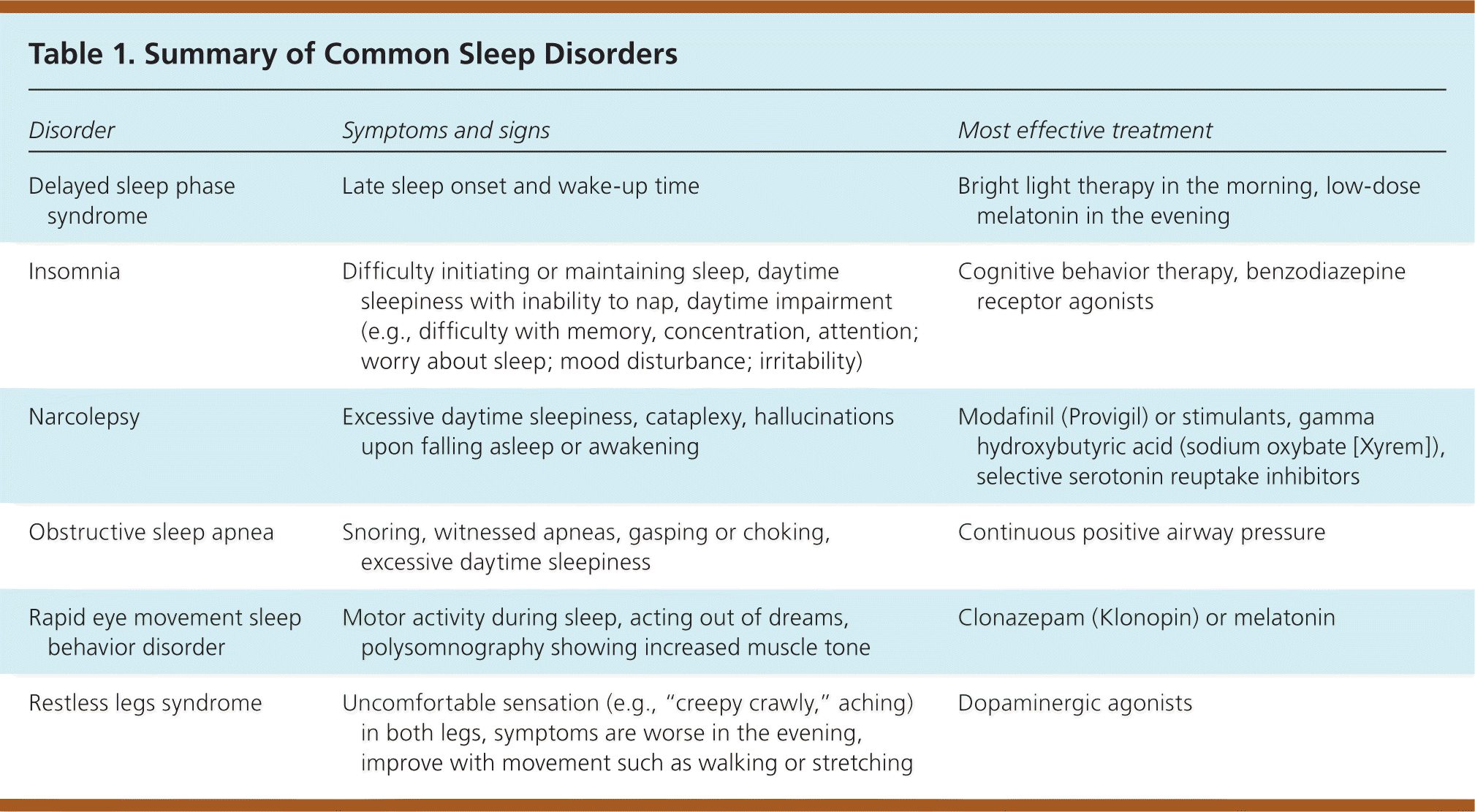
In addition, CBT drop-out rates range from 22% to 30%. Given the inherent selection bias in study populations consenting to enroll in CBT research, real-life CBT completion rates could be well over-estimated. Nonetheless, between 19% and 26% of insomnia patients fail to show any response to CBT-I and the effect size of CBT in insomnia is far less than that of CBT for anxiety, post-traumatic stress disorder (PTSD), depression, or panic disorder. In the interest of increasing access and reducing cost, many groups have developed simplified or abbreviated versions of CBT for insomnia, organized training programs for advanced master’s level providers including nurse practitioners and physician assistants, and/or using technology, such as Interned-based programs. 
Despite the strong recommendations adopted by sleep societies for CBT in treating insomnia, not all sleep clinics offer CBT. The two major barriers to more widespread use of CBT are the lack of CBT expertise and the limited awareness of its efficacy. While a detailed analysis of its efficacy and effectiveness is beyond the scope of this review, there are instances when CBT may not be a robust enough treatment to reduce symptoms of insomnia or practical enough to be applied universally. We will also identify opportunities for future research to further this important area of medicine.Ģ. Cognitive behavioral therapy limitationsĬBT is a non-pharmacologic intervention designed to modify learned-behavioral maladaptation to aberrant sleep patterns. This review is intended to lay out the rationale behind prescribing hypnotics for insomnia and to provide guidance on drug selection. The specificity and the chronicity of the patient’s sleep complaint as well as the presence of concomitant medical and/or psychiatric comorbid conditions should guide the prescribing provider in choosing the appropriate hypnotic agent. Faced with these scenarios, a variety of pharmacological agents are used by physicians to treat this disorder, including those agents approved by the Food and Drug Administration (FDA) for insomnia, as well as medications that have sedating properties, but have not been systematically studied for their effectiveness in randomized controlled trials. 
Realistically, however, only a third of patients with insomnia experience full remission and a significant proportion experience residual sleepiness following CBT. CBT has many advantages over hypnotics including fewer side effects, more cost-effective, and safer to use during pregnancy and breastfeeding. Further, these studies have demonstrated that CBT performs as well as pharmacotherapy or even slightly better in the short term, with superior results in the long term. Prior meta-analyses have shown that CBT is an efficacious treatment for reducing sleep latency, wake time after sleep onset, and early morning awakenings, as well as increasing sleep efficiency. Addressing these behavioral aspects should be the first step toward a satisfactory response. Although hypnotic medications are indicated in situational insomnia, psychological and behavioral factors are almost always an integral component of persistent insomnia. The two widely practiced treatment modalities for insomnia are cognitive behavioral therapy (CBT) and pharmacotherapy. Conservative estimates of the total direct cost to the US economy ranges between 1 USD.9 billion to 92 USD.5 billion annually. In addition to accounting for 5 million doctor visits annually, untreated insomnia is financially costly in its associated loss of work-place productivity, increased absenteeism, and work-related accidents. 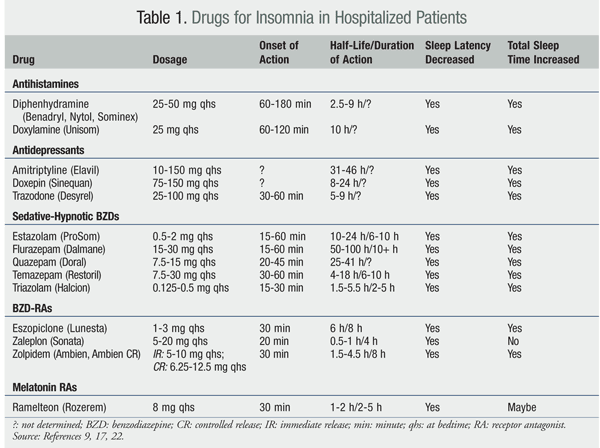
Insomnia has been consistently associated with problems with cognitive function, impaired mental health and poor health-related quality of life. According to WHO data, insomnia ranked 11th in the list of most important brain disorders with respect to global burden. It is the second most common psychological health problem, affecting one in three adults in the United States and 10% to 15% of people worldwide. Insomnia is one of the most prevalent sleep disorders worldwide.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
